Biomechanics and Histopathology: The Physiological Impact of Removable Dentures
In the discipline of oral prosthodontics, the application of removable dentures represents a significant alteration to the oral homeostasis. Unlike fixed prostheses which transmit masticatory forces via the periodontal ligament (PDL) to the alveolar bone, removable dentures transmit these forces directly through the mucoperiosteum. This fundamental shift in load transfer initiates a cascade of biological responses within the supporting tissues. From an academic perspective, as analyzed by The Gentle Care Hub, evaluating the efficacy and biological cost of these prostheses requires a rigorous analysis of residual ridge resorption (RRR), mucosal histopathology, and the microbial ecology of the acrylic substrate. The interface between the polymethyl methacrylate (PMMA) base and the living epithelium is a site of constant biological interaction, governed by the principles of pressure, friction, and biofilm dynamics.
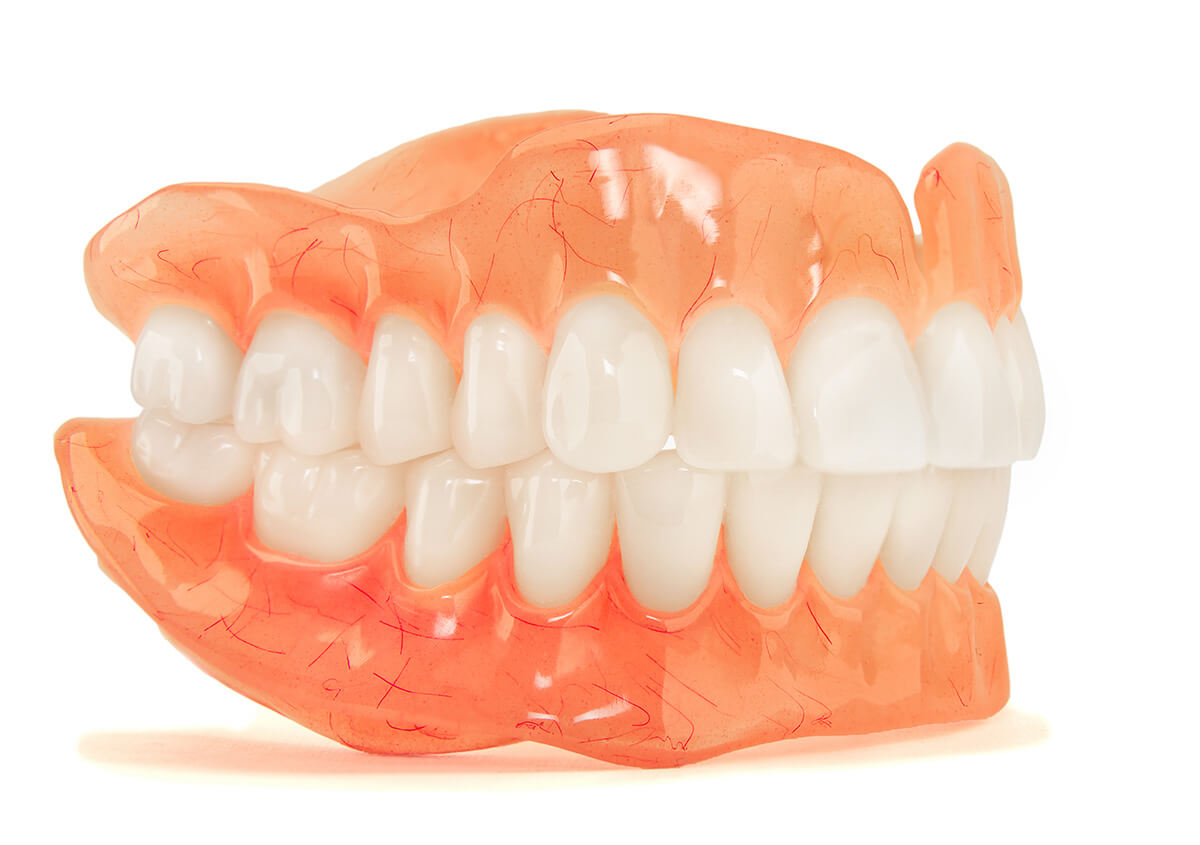
Biomechanics of Removable Dentures on Alveolar Bone
The most critical physiological consequence of edentulism rehabilitated with removable dentures is the progressive atrophy of the alveolar ridge. The alveolar bone is functionally dependent on the tensile stimulation provided by the Sharpey’s fibers of the PDL.
Osteoclastic Activation via Compression
When teeth are extracted and replaced with removable dentures, the mode of mechanical stimulation shifts from tension to compression. According to Wolff's Law, bone remodels in response to the loads placed upon it. However, the mucoperiosteum is not designed to bear the full load of mastication. The compressive forces exerted by the denture base restrict blood supply to the underlying periosteum, creating localized hypoxia. This hypoxic environment upregulates the recruitment of osteoclasts, leading to the resorption of the underlying cortical and cancellous bone. This phenomenon is particularly pronounced in the mandible, where the available surface area for load distribution is significantly less than in the maxilla. The rate of resorption is continuous and irreversible, often exacerbated by ill-fitting prostheses that create focal pressure points rather than distributing load hydrostatically.
Mucosal Histopathology Under Removable Dentures
The soft tissue response to a removable prosthesis varies from physiological adaptation to pathological inflammation. The oral mucosa must adapt to the mechanical friction of the acrylic base.
Hyperkeratosis and Acanthosis
In a well-adapted prosthesis, the epithelium may undergo hyperkeratosis—a thickening of the keratin layer—as a protective mechanism against friction. However, aberrant loading patterns frequently lead to pathological changes. Chronic irritation from removable dentures can induce traumatic ulcers (decubitus ulcers) or fibrous hyperplasia (epulis fissuratum). Histologically, these lesions show a proliferation of fibroblasts and an infiltration of chronic inflammatory cells. Furthermore, the occlusion of the salivary ducts by the denture base can alter the viscosity and buffering capacity of the saliva film, reducing the mucosal defense against mechanical trauma. The tissue health is directly correlated to the stability of the denture base; instability results in shear forces that strip the epithelial barrier, leading to chronic sub-prosthetic inflammation.
Denture Stomatitis and Microbial Ecology
The acrylic surface of removable dentures provides a distinct ecological niche for oral microbiota, specifically Candida albicans.
Biofilm Adhesion to PMMA
Polymethyl methacrylate (PMMA) is inherently porous on a microscopic scale. These micropores serve as reservoirs for fungal colonization. In the presence of a prosthesis, the oral environment between the palate and the denture base becomes anaerobic and acidic, favoring the proliferation of Candida. This condition, known as Denture Stomatitis (Newton’s classification types I, II, and III), is characterized by erythema and edema of the palatal mucosa. It is not merely a surface infection; fungal hyphae can penetrate the porous acrylic and, in severe cases, invade the superficial layers of the epithelium. The presence of removable dentures disrupts the natural cleansing action of the tongue and saliva, necessitating rigorous chemical disinfection protocols to manage the biofilm load and prevent chronic mucosal inflammation.
The transition to removable dentures involves a significant reorganization of the neuromuscular system.
Neuromuscular Adaptation and Proprioception
Loss of Periodontal Mechanoreceptors
Natural teeth are equipped with mechanoreceptors in the PDL that provide exquisite tactile sensitivity and proprioceptive feedback, regulating bite force and jaw position. Upon extraction, these receptors are lost. The patient must rely on osseoperception and mucosal mechanoreceptors, which have a much higher threshold for firing. This results in a reduced masticatory efficiency—often only 20-30% of natural dentition. The central nervous system must create new engrams (muscle memory patterns) to control the mandibular movements required to stabilize the removable dentures during function. This neuromuscular adaptation is a biological learning process, heavily influenced by the patient’s age and neuroplasticity.
Fundamentally, understanding what are removable dentures requires recognizing them as a biological compromise. While they restore esthetics and limited function, they impose non-physiological compressive loads that accelerate bone resorption and alter the microbial landscape of the oral cavity. Understanding these micro-level mechanisms is essential for the clinician to minimize iatrogenic damage and preserve the remaining oral structures for as long as possible.
